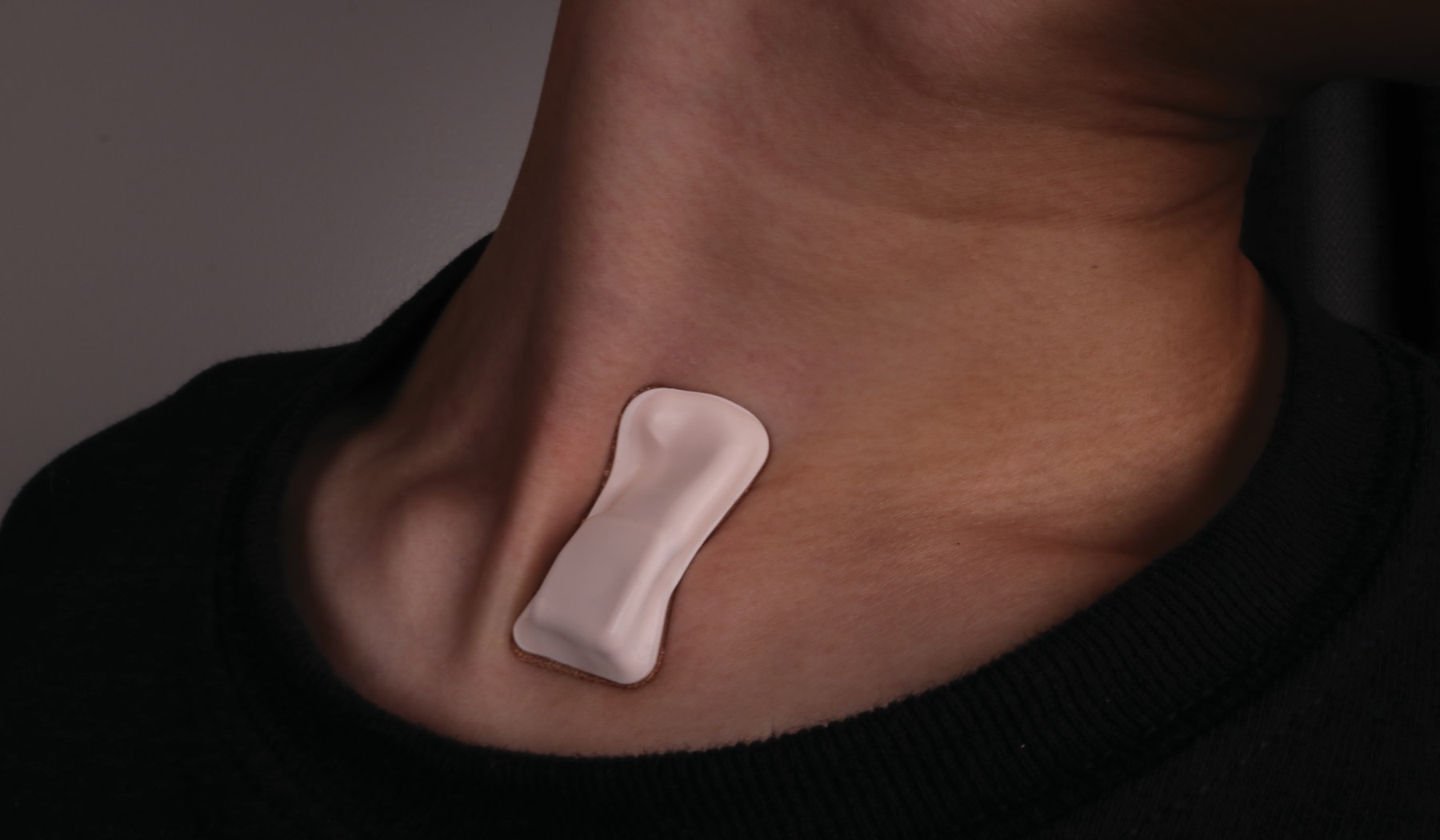
An adhesive sensor much like a Band-Aid has been developed by Northwestern University to monitor for early signs of COVID-19 infection when connected wirelessly to an iPad.
Announced Monday, the device sticks to the throat and looks for coughing and various onset symptoms of COVID-19 to aid treatment of patients with the deadly virus.
Northwestern University said the device could prove particularly valuable as a way to diagnose COVID-19 in health care workers by detecting symptoms at an early stage.
About 25 affected individuals began using the devices two weeks ago. The patients are being monitored both in the clinic and at home. So far, more than 1,500 cumulative hours of monitoring have generated more than 1 terabyte of data. Part of the statement read:
“Capable of being worn 24/7, the device produces continuous streams of data and uses artificial intelligence to uncover subtle, but potentially life-saving, insights. Filling a vital data gap, it continuously measures and interprets coughing and respiratory activity in ways that are impossible with traditional monitoring systems.”
COVID-19 symptom sensors
About the size of a postage stamp, the soft, flexible wireless device sits at the base of the throat. From there, it monitors patterns in the throat and chest, looking for irregular or labored breathing. Additionally, the device checks for respiratory sounds, heart rate and body temperature.
Researchers hope that over time, using new data already being collected, the device could pick up COVID-19 trends before workers notice them. This could provide an opportunity to engage in appropriate precautionary measures and to spur further testing as quickly as possible.

Photo: Northwestern University
The adhesive device automatically syncs to a nearby iPad once a day when it is removed to be charged. (It does not currently offer real-time data while connected to the patient.) From there, the data is uploaded to the cloud and examined using an artificial intelligence algorithm. The software searches for symptoms related to COVID-19.
“We anticipate that the advanced algorithms we are developing will extract COVID-like signs and symptoms from the raw data insights and symptoms even before individuals may perceive them,” said Arun Jayaraman, a research scientist at Shirley Ryan AbilityLab who is leading the algorithm development. “These sensors have the potential to unlock information that will protect frontline medical workers and patients alike — informing interventions in a timely manner to reduce the risk of transmission and increase the likelihood of better outcomes.”
The device, capable of being worn 24/7, has no external ports for power or connectivity, making it easier to disinfect.